Reception: ![]() +36/30 show
+36/30 show
6721 Szeged, Osztrovszky utca 12.
Open every week-day since 1996
Open on week-days from 8 AM to 9 PM
24 578 satisfied customers
Serving you since 1996
Gum disease or periodontitis is a surreptitious disease affecting the health of your teeth. It often goes unnoticed as patients tend to ignore small signs like bleeding gums. These small signs should be seen as early warning that something is wrong with one’s teeth. In this chapter, we would like to help you recognise these signs so you can see a dentist in time and keep your natural teeth.
The following signs indicate that you have gum disease:
If you recognise these symptoms, it is a good idea to see a periodontist – a specialist in the treatment of periodontal diseases – as soon as possible.
vissza a kérdésekhez
When we eat, a thin biofilm called plaque forms on the surface of our teeth. Plaque is a rich breeding ground for the bacteria living in the mouth. If we do not clean our teeth and the gaps between them thoroughly, this thin layer of plaque hardens over time, forming tartar. Tartar harbours bacteria that induce gum inflammation. As a consequence, the gum swells and de-taches from the surface of the tooth, opening up the way for further bacterial ingress. Patho-gens get lodged in between the tooth and the gum and also induce inflammation. This leads to the necrosis of the tissues surrounding the tooth and the formation of so-called periodontal pockets.
The resulting condition is called periodontitis or gum disease, and it comes with an unpleasant symptom: bad breath. At this stage, seeing a periodontist is a must in order to prevent the in-flammation from spreading to the bone tissue of the jaw. Unless the condition is treated, the structure supporting the teeth weakens and the teeth become loose, shift out of position, or even fall out.
vissza a kérdésekhez
There are four factors that play into the development of gum diseases:
vissza a kérdésekhez

Gum disease and its consequences are major risk factors not only in terms of our teeth but also in terms of our overall health. The bacteria involved in gum disease also produce toxins that harm blood vessels. International studies clearly suggest a relationship between this effect on the one hand and heart failure, stroke, and premature births on the other.
It is possible to prevent these risks. When it comes to gum diseases, health awareness and ap-propriate home oral hygiene are key. Of course, our overall lifestyle, nutrition, and possible bad habits (such as, for example, smoking) also contribute significantly to gum problems.
vissza a kérdésekhez
If detected in time, the progress of gum disease can be reversed. In more severe cases, it can be stopped and treated. There are several ways to successfully treat gum disease:
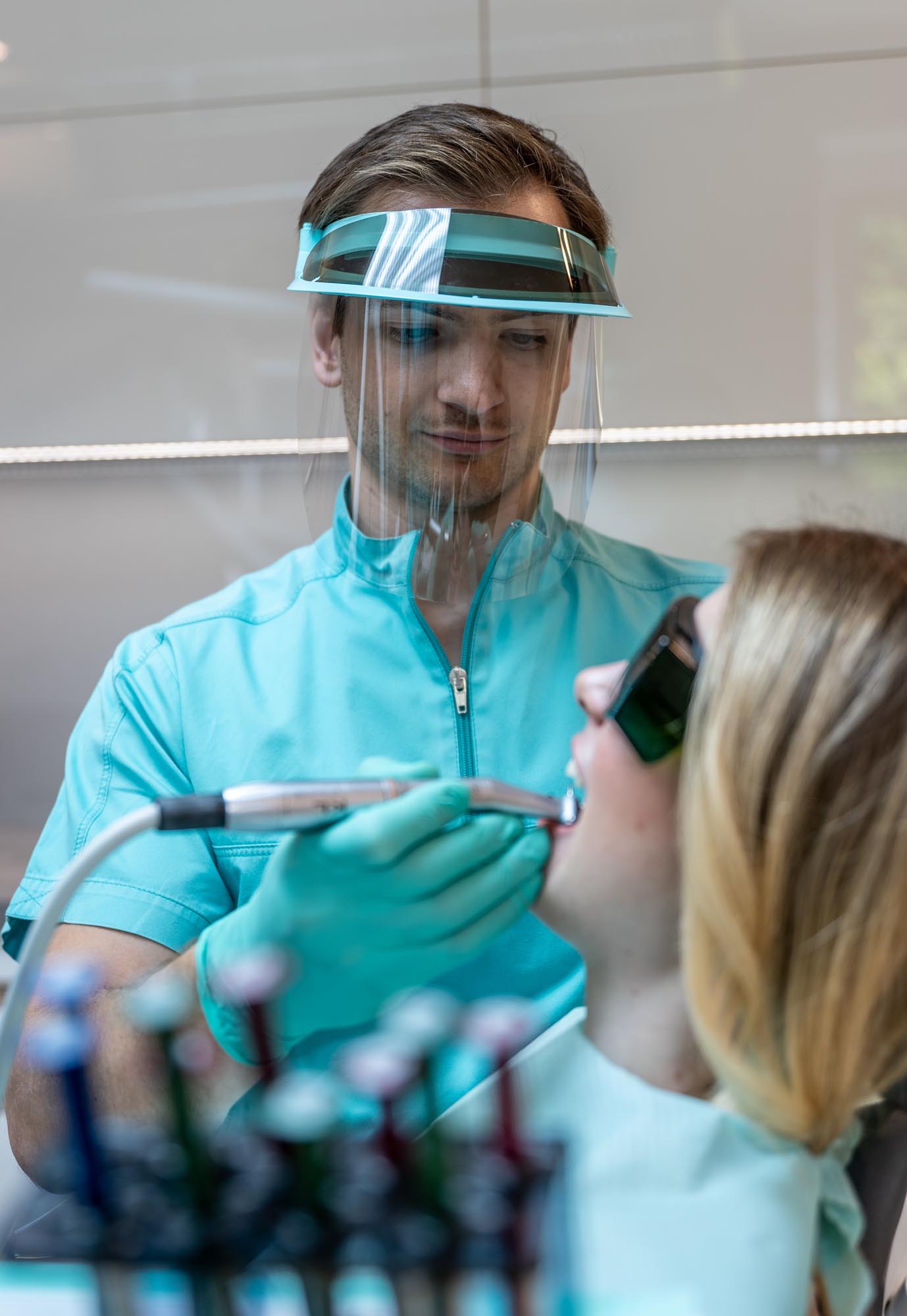
When it comes to gum disease, time is very important.
The sooner you see a specialist the eas-ier it is to stop and reverse the progress of gum disease.
Call +36 30 206 9532 and ask for a consultation appointment for periodontal screening in our dental clinic in down-town Szeged and prevent the unpleasant consequences of gum disease!
We look forward to seeing you!
vissza a kérdésekhez